Edward Cho
Seeing Without Recognizing: The Hidden Reality of
Prosopagnosia
You enter school, and you give a friendly greeting to someone you think is your friend. They look back at you with an expression of confusion. Later in the day, your true friend comes over to you, upset with you because of your apparent lack of acknowledgement of them. However, imagine this is every single day of your life, not because of your own forgetfulness or
inattentiveness, but because your brain is literally incapable of recognizing faces. For people with prosopagnosia, also referred to as face blindness, this is their reality. It is defined as “a disorder of facial recognition in which an individual is unable to recognize faces despite normal intelligence and without any apparent brain damage.”
What Is Prosopagnosia?
The definition of Prosopagnosia is “a defect in recognizing faces despite normal vision, memory, and intelligence” (National Institute of Neurological Disorders and Stroke [NINDS], 2023). Individuals with Prosopagnosia have normal vision, but they cannot recognize faces. They have no problem seeing faces; they just do not know whose faces they are seeing. There are two types of Prosopagnosia: One is caused by an injury, such as a stroke. This is known as Acquired Prosopagnosia. The second type is known as Developmental Prosopagnosia. This is caused by no known damage to the brain. Neuroscientific studies have located the fusiform face area (FFA), which is responsible for facial recognition. Damage to this part of the brain is linked with Prosopagnosia (Kanwisher & Yovel, 2006).
How Common Is It?
While prosopagnosia is often regarded as an uncommon phenomenon, it is more prevalent than people might think.
Figure 1. Visual representation of the estimated prevalence of prosopagnosia in the general population (based on Bowles et al., 2009).
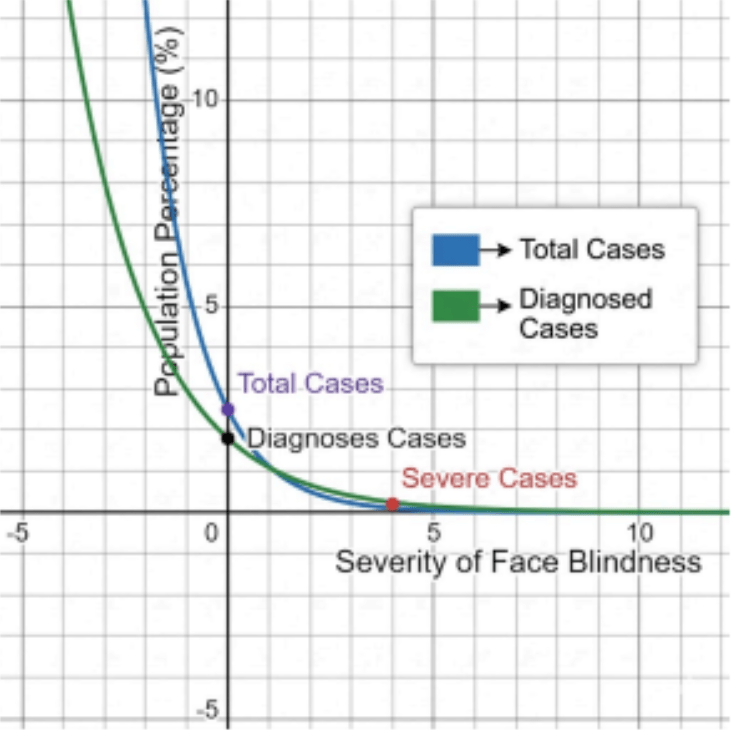
The above graph represents an important distinction in the prevalence of face blindness and how it is perceived in society, which brings us to the “Diagnosis Gap.” The Prevalence Spectrum: The blue line represents the “Total Cases” of face blindness in society, and it is clear that a large portion of the population is dealing with some level of face blindness. As the level of face blindness is increased (i.e., moving further to the right along the x-axis), the total number of people dealing with the problem decreases significantly.
The Identification Lag: The green line represents the “Diagnosed Cases” of face blindness in society, and it is quite clear that the number of people who have actually sought and received a medical diagnosis of face blindness is significantly lower than the actual number of people dealing with the problem. The line is relatively flat in comparison to the total cases line when dealing with mild and moderate face blindness.
Severe Cases: It is only when moving to the far right of the graph, the “Severe Cases” (represented by the red dot), that the lines converge and indicate that only in these extreme cases is face blindness being recognized by professionals.
Research
It is estimated that 2-2.5% of people in society suffer from some level of prosopagnosia. Severe cases of face blindness only affect 0.1-0.3% of people in society. It is also estimated that people who suffer from face blindness often do not know that they are dealing with face blindness and often attribute their problems to having a bad memory. Given the numbers, in an average high school of 2,000 students, 40-50 of them could be dealing with face blindness.
The Science Behind Face Recognition
Facial recognition is not a simple visual task—it is a highly specialized neurological process. The brain rapidly analyzes:
– Spatial relationships between facial features.
– Subtle differences in shape and symmetry.
– Emotional expressions and movement.
In people with prosopagnosia, this system does not function normally. Functional MRI studies show reduced or absent activation in the fusiform face area when viewing faces (Kanwisher & Yovel, 2006). Interestingly, many individuals with prosopagnosia can still recognize objects, read, and even identify emotions from voices, showing that the deficit is highly specific to faces.
Daily Life and Social Impact
The effects of prosopagnosia extend far beyond simple inconvenience. Social interaction becomes unpredictable and often stressful. A study by Yardley et al. (2008) found that individuals with prosopagnosia frequently report:
– Social anxiety and embarrassment.
– Fear of offending others.
– Difficulty forming relationships.
Some people even struggle to recognize their own reflection or identify family members in photos. In extreme cases, individuals rely almost entirely on non-facial cues such as voice, posture, or clothing.
Coping Strategies
Despite these challenges, many individuals adapt remarkably well. Common strategies include:
– Memorizing voices and speech patterns.
– Recognizing hairstyles, clothing, or accessories.
– Using context (location, expected people).
– Relying on technology such as labeled photos or contact apps.
However, these strategies can fail in situations where context changes—such as seeing a teacher at a grocery store or a friend with a new haircut.
Can It Be Treated?
At present, there is no definite cure available for the disorder of prosopagnosia. However, some studies have indicated that certain interventions might help improve the capacity of facial recognition by enhancing skills in holistic processing. According to DeGutis et al.’s (2014) study, training programs might be helpful in improving facial recognition capacity by enhancing skills in holistic processing.
Why Prosopagnosia Matters
Prosopagnosia reveals how complex and specialized the human brain truly is. It challenges the assumption that recognizing faces is automatic and universal. Beyond its medical significance, the condition has broader implications:
– It informs research in neuroscience and cognition.
– It influences the development of facial recognition technology.
– It highlights the importance of neurodiversity and invisible conditions.
Understanding prosopagnosia also encourages empathy. What may appear as rudeness or indifference could actually be a neurological limitation.
Conclusion
Prosopagnosia is not simply the inability to recognize faces; it is a state that fundamentally changes the manner in which people interact in society. The personal nature of prosopagnosia is often misunderstood and has significant implications for social interactions and relationships. However, as awareness and technology continue to progress, there is hope for those suffering
from prosopagnosia. Until then, it is crucial to recognize prosopagnosia as a condition and understand that, at times, it is not simply about not being able to see something; it is about understanding something that others cannot.
References
Bowles, D. C., McKone, E., Dawel, A., Duchaine, B., Palermo, R., Schmalzl, L., … & Yovel, G. (2009). Diagnosing prosopagnosia: Effects of ageing, sex, and participant–stimulus ethnic match on the Cambridge Face Memory Test and Cambridge Face Perception Test. Cognitive Neuropsychology, 26(5), 423–455. https://doi.org/10.1080/02643290903343149
DeGutis, J., Cohan, S., & Nakayama, K. (2014). Holistic face training enhances face processing in developmental prosopagnosia. Brain, 137(6), 1781–1798.
https://doi.org/10.1093/brain/awu062
Kanwisher, N., & Yovel, G. (2006). The fusiform face area: A cortical region specialized for face perception. Philosophical Transactions of the Royal Society B, 361(1476), 2109–2128. https://doi.org/10.1098/rstb.2006.1934\
Lewis, J. G. (2013, September 23). Prosopagnosia: Why some are blind to faces. Psychology Today. https://www.psychologytoday.com/us/blog/brain-babble/201309/prosopagnosia-why-some-are-blind-to-faces
National Institute of Neurological Disorders and Stroke. (2023). Prosopagnosia information page. https://www.ninds.nih.gov
Yardley, L., McDermott, L., Pisarski, S., Duchaine, B., & Nakayama, K. (2008). Psychosocial consequences of developmental prosopagnosia: A problem of recognition. Journal of Psychosomatic Research, 65(5), 445–451. https://doi.org/10.1016/j.jpsychores.2008.03.013